If you’ve had lymph nodes removed as a result of breast cancer surgeries, you could be at risk for a condition called lymphedema. It's important to know what it is, what the symptoms are and how to treat it. Because, like all things breast cancer, early detection and management will impact your long-term outcome.
Lymphedema can feel like a pretty unfair side effect of life-saving cancer treatments, but know you are not alone in this struggle. At Stage, we are encouraged by the newer developments that are emerging in the field of lymphedema prevention and management. Our goal is to empower you with information and resources to help you navigate this condition as you’ll see below!
What is the lymphatic system?
The lymphatic system is a circulatory system that’s made up of lymph fluid, lymph vessels and lymph nodes. Part of the immune system, the lymphatic system’s role is to fight infection and other diseases in the body. Simply put, the lymphatic system acts like a superhighway that transports and removes waste and toxins from the various regions of the body (arms, legs, stomach, neck, etc.), helping to fight infection.
What is ‘lymph’?
Lymph is a clear fluid containing white blood cells that fight germs, abnormal cells (like cancer cells), foreign substances and infection. The lymph collects waste, bacteria and damaged cells from inside the body’s tissues so that they can be removed or destroyed. Lymph drains into lymph vessels that carry it to lymph nodes. Lymph nodes clean the lymph fluid and add more white blood cells to it.
What are lymph vessels?
Think of lymph vessels as tubes that transport lymph fluid throughout the body to lymph nodes and back to the veins just below the collarbone (called subclavian veins). The network of lymph vessels are similar to blood vessels that carry blood. Lymph vessels carry waste products, germs and damaged cells away from the body’s tissues.
What are lymph nodes?
Lymph nodes are small bean-shaped structures that connect the lymph vessels and play a crucial role in the functioning of the lymphatic system. You have roughly 600 lymph nodes in your body; there are clusters of them in your neck, armpits, abdomen and groin, around your elbows, behind the knees and under the jaw and chin. Lymph nodes act as a filtration system to move or flush waste and toxins out of a given region of the body and to fight infection. That’s why you can feel pain and swelling surrounding your lymph nodes when fighting off a cold or infection — your lymph nodes are working extra hard to keep up with excess waste and illness. The removal of as few as 1 lymph node from an area of the body can compromise the functioning of the lymph system — meaning the lymph system has to learn how to re-route the fluid to nearby lymph nodes to drain waste from an area. This can take time and doesn’t always work.
What is lymphedema?
Lymphedema is a condition that can occur when lymph fluid is backed up or trapped in a certain region of the body. It presents as swelling or fullness. In breast cancer patients, lymphedema most commonly occurs in the arms or chest wall on the side where cancer treatment occurs. If you’ve had an axillary node dissection or even 1 lymph node removed in your armpit, you are at risk for lymphedema occurring in your arm on the affected side. Having radiation can also damage your lymphatic system, further increasing your risk for lymphedema.
What are the signs and symptoms of lymphedema?
- Swelling: When lymphatic drainage malfunctions or is compromised, fluid accumulates in the affected area. This becomes more noticeable the more advanced the condition becomes. Swelling can be reduced or mitigated through the use of compression garments, manual lymphatic drainage, exercise and other physical therapy interventions. It's important to address the swelling as soon as you notice it, for the best chance of reversing it. In some cases, the swelling becomes permanent — and no one wants that! The swelling can be painful, cause your garments to fit incorrectly and, in some cases, can become infected.
- Heaviness: When swelling occurs in the fingers, arm, chest wall it can feel like a dull ache, fullness or pressure.
- Restricted range of motion or stiff joints
- Redness or itching in the affected area
- Hardening or thickening of skin
Common misconceptions
-
Cording: Cording (or axillary web syndrome, AWS) is a condition that can occur right after your breast cancer surgery, where the lymph fluid gets trapped in the lymph channels that run through your arm and connect all the way through your ribs to your stomach. This may feel like a tight rubber band within your arm or armpit and look like strings or tendons below the skin. It will feel tight and can restrict your range of motion for movement. Physical therapy, massage and stretching can alleviate this condition. If you’re experiencing it, let your breast surgeon know and they can refer you to a physical therapist that is trained in your condition.
While cording is a common side effect in patients who have had lymph node removal surgery, it is not a sign of lymphedema.
What health problems can lymphedema cause?
- Lymphedema can result in serious bacterial infections, including cellulitis, which can be painful to the touch and require hospitalization for treatment. If you experience redness and hotness in the affected limb, chills or fever, you may have an infection that is spreading rapidly. Seek immediate medical treatment.
- Wounds may heal more slowly in the limb affected by lymphedema — take extra precaution to protect it from bug bites and cuts.
- Changes in the size of your limbs from lymphedema may lead to ill-fitting clothes. You may feel depressed, ashamed, upset or angered by these changes.
- Lymphedema may lead to joint stiffness or soreness in the affected part of the body.
How long does lymphedema last?
Unfortunately, there is no cure for lymphedema. The best course of action is prevention. Moreover, the lymphatic system can ebb and flow and often be unpredictable. In my experience, sometimes my condition responds well to wearing compression garments and self massage, and other times it doesn't. This can be incredibly frustrating. Regardless, it's important to know the options for managing your condition both at home and with the help of a qualified physical therapist or lymphatic masseuse.
Things that can trigger the onset of lymphedema:
Anything that causes injury to the lymphatic vessels below the skin can increase your risk of developing lymphedema, or having a flare-up.
- Breast cancer surgeries: Mastectomy, lumpectomy, lymph node removal or reconstruction
- Radiation: Scar tissue from radiation therapy can press on the lymph vessels, compromising their function
- Being overweight: Extra fat can put pressure on the lymph nodes and vessels, making it harder for fluid to flow
- Infections caused by bug bites or injuries to the affected area
- Air travel: While recent research suggests that air travel may not increase the risk of the onset of lymphedema, changes in air pressure can cause lymphedema flare ups
Note: there is conflicting guidance on the whether to avoid getting blood drawn, an IV or blood pressure taken on the affected arm if you’ve had an axillary node dissection. I’ve also received conflicting guidance on whether acupuncture is ok to have in the affected area. Always check with your surgeon or oncologist to assess your individual risk factors before proceeding.
Lymphedema staging
- Stage 0: Subclinical/Latent. There are no signs and symptoms, but there is abnormal flow in the lymphatic system. At this stage there can be detection with a lymphoscintigraphy study. You can be at Stage 0 for years before symptoms or pain develop.
- Stage 1: Early, mild lymphedema. Accumulation of fluid and swelling begins to happen, but resolves with elevation, massage and compression. Pressing on the area may leave a dent, which is called “pitting.”
- Stage 2: Moderate. Permanent swelling that does not resolve with elevation, massage and compression. Pressing on the area no longer leaves a dent, and skin changes such as thickening and scarring occur.
- Stage 3: Advanced. In this stage, the limb becomes large and misshapen (a.k.a. elephantiasis), skin has thickened with “wart-like” growths and extensive scarring. Stage 3 is rare in breast cancer patients.
Prevention, treatment & mitigation tactics
The following modalities can be used to prevent, improve or, in some cases, reverse lymphedema that may have occurred following the removal of lymph nodes as part of your breast cancer treatment. At a minimum, if practiced regularly, you can keep your condition from getting worse.
Compression garments: These will become your best friend, your security blanket. Compression garments come in all kinds of colors and patterns. Note it is recommended to wear a compression sleeve to support your lymphatic system in the following conditions:- When flying on a plane or traveling to high-altitude areas (yes, that means while you’re skiing).
- When exercising or doing manual labor, particularly when you are walking or hiking as the arms are swinging downward and lifting weights. It’s best to wear them during exercise, cleaning the house or gardening. If it bothers you too much during the activity, you can put it on for several hours after finishing the activity (according to my physical therapist, but opinions may differ among practitioners, so always check with a professional before deciding what’s right for you).
- While doing computer work
Work with your surgeon for a referral to a specialist who can measure your arm for the right compression garments (sleeve, glove, gauntlet, bras, tank tops, etc.) and help you order the right product for you. It's also possible to have the garments custom-made. This can be costly, but starting in 2024, Medicare and Medicaid insurances will be required to cover compression garments; it is expected that most insurances will follow suit thereafter. (Give it up for small victories!) For more advanced cases of lymphedema, you may find benefit in using a night garment as well; these are different from daytime garments and have padding or quilting built into them.
Nutrition: It is recommended that those experiencing, or at risk for, lymphedema avoid foods that are high in saturated fats and sugar and incorporate whole foods into their diets. Refined grains, chemically modified fats and most animal/dairy products should be avoided as they are often processed with additives or high amounts of salt, which can exacerbate lymphedema symptoms.
Hydration: Dehydration can slow down the lymphatic system function, so drinking plenty of water and eating foods with high water content are recommended. Caffeine and alcohol should be limited accordingly.
Hygiene: Keep the arm clean and moisturized.
Avoid insect bites: Use bug spray when outdoors in areas prone to mosquitos and other pesky insects. For a natural non-toxic bug repellent option look for formulas made with natural ingredients like lemongrass. If you do get an insect bite, clean and disinfect it right away to avoid an infection.
Avoid extreme temperatures and sunburns: Heat causes the blood vessels to dilate and more fluid to flow into your tissues. If you have lymphedema or are at risk of developing it, check with your physician to confirm safety before using steam rooms, saunas or jacuzzis and taking hot baths. If deemed safe, it is recommended to limit exposure to 15 minutes or less and to keep the affected limb out of the water, if possible. Prolonged sun exposure is also to be avoided; use sunscreen when exercising outdoors or sunbathing to reduce your risk of sunburn, which can contribute to swelling.
Physical Therapy: There are a wide range of modalities (referred to as complete decongestive therapy) a trained lymphedema physical therapist can employ while working with you. Most of them can be performed at home once you’ve been trained in the proper technique, which will be important for long-term maintenance of your condition:
Lymph drainage massage: This involves activating the lymph nodes using circular motions around the collar bone, neck, abdomen and armpits. This is followed by sweeping motions up the arm and/or along the chest wall and across the back to help guide any stagnant lymph fluid to nearby healthy nodes. Since the lymph system is just below the surface, it's a light pressure massage with short strokes. Some helpful tutorial videos can be found here.
Kinesiology taping: This can help alleviate pain, enhance muscle function, aid joint positioning, and clear lymph that is pooling under the skin. It works by creating space between the muscle and skin, which enables the blood and lymph to flow more freely in the affected area. Kinesiology taping is waterproof and can be worn for 1-3 days or longer. It's best to work with a therapist to do this the first time, before attempting to do it at home. To give you an idea of what’s involved, a helpful self-tutorial can be found here.
Wrapping: In this option, your therapist will use short stretch bandages, gauze, tape and possibly foam to wrap your arm. This is done for a few weeks initially to reduce swelling before transitioning into a compression garment. Here’s a self-wrapping video to give an idea of what’s involved. Again, we recommend working with a therapist to tailor the wrapping approach to your needs.
Cupping: An ancient healing technique that originated in Asia, cupping is used to ease pain, increase or decrease blood flow to a given area of the body and to promote healing. Your provider will place cups on your back, chest wall, arm or other parts of your body. A vacuum or suction force inside the cup pulls your skin upward. Therapists are starting to use cupping to break up scar tissue and possibly promote restoration of nerve sensation in mastectomy patients. This is new and not well studied, so ask your therapist if this could be right for you.
Laser treatment: This painless, low-level treatment can be done by a trained therapist in-office. Laser treatment can help reduce arm volume, restore function in the lymph vessels, improve range of motion and help to soften fibrotic tissue.
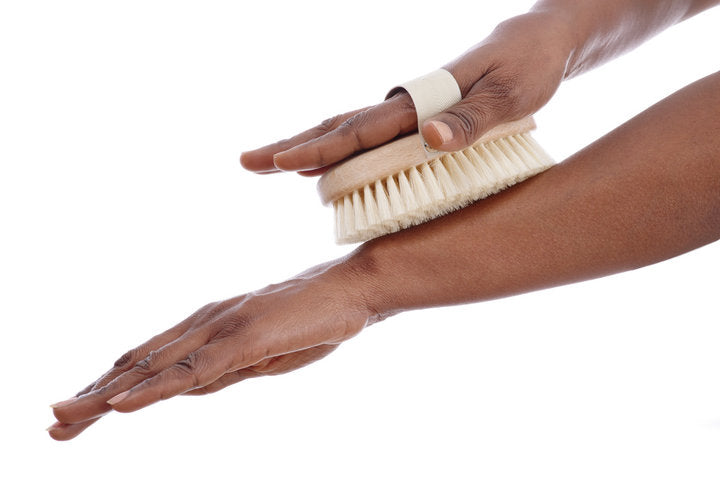
Dry Brushing: This ancient Eastern technique helps to stimulate the movement of lymphatic fluid in the body. Dry brushing is best done on dry skin before showering using the same pattern of sweeping motions used in lymphatic draining massage. Another helpful video can be found here. It is important to know that dry brushing is not well studied for lymphedema, but can be very helpful in some patients.
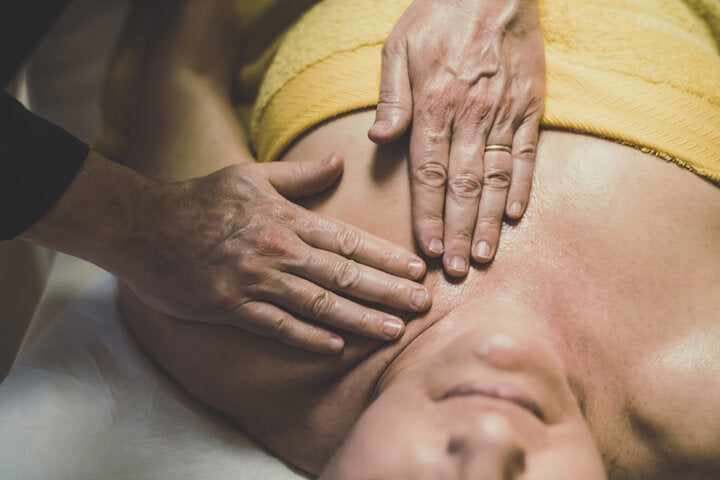
A note on traditional massage:
While a spa day can do wonders to ease the mind, you must exercise caution when getting a traditional massage (i.e. Swedish, relaxation, deep tissue, hot stone). If you’ve had lymph nodes removed, inform your therapist that only very light touch should be used on the affected arm and underarm area. If you have lymphedema, traditional massage should be avoided in the affected area altogether.
Lymphedema Pumps: There are two types of lymphedema pumps that are widely prescribed for at-home use. Both technologies have been proven to reduce limb volume in lymphedema patients.
- Pneumatic pumps: These devices use an air-based pumping technology that’s been around for 30 years. They come with garments for the limb, trunk and groin that connect via hoses to the electronic base. The 4 major brands are Tactile Medical, Airos Medical , Lymphapress, and Biotab Compression.
- Non-pneumatic pump: The Koya Dayspring pump is a newer technology that’s non-pneumatic (airless), mobile and portable for use at home or while traveling.
Exercise and Stretching: Swimming, rebounding on a trampoline or exercise ball and yoga have all been recommended to me by my therapists to stimulate lymph flow. I find that doing yoga twice a week really helps keep my cording at bay. Strength training is also recommended, especially if you were active before developing lymphedema. It's best to wear your compression garments during exercise and pay attention to any new swelling as you might need to ease up and adjust your routine. Work with your physical therapist for any questions. Many cancer centers have free exercise programs, so check what may be available to you.
Lymphovenous bypass surgery (LVA): This minimally invasive microsurgical procedure involves rerouting clogged lymph vessels to nearby veins as a method of draining stagnant lymph fluid in the extremities. This is a newer field of medicine and is most successful when performed in the earlier stages of lymphedema (1-2), or even preventatively at the time of the Axillary Node Dissection. If you have fibrotic tissue (fat deposits) that have formed in the affected area, your surgeon may offer liposuction to remove the excess tissue, also known as a debulking surgery. This is also an outpatient procedure. Some surgeons will perform the two procedures in the same surgery, but newer research out of the Cleveland Clinic is showing more favorable long-term results by tackling them one at a time. Discuss the pros and cons of both approaches with your surgeon to determine the best course of action for you.
Lymph node transfer surgery: In this procedure, lymph nodes are harvested from an area where you have a cluster of nodes (like the groin, above the collarbone, below the chin or around the abdomen) and transferred to the axilla area in the armpit to restore lymph flow to the arm and affected region. This is a more invasive procedure and does come with some risk of a secondary lymphedema developing in the area of the donor site. For that reason, it's reserved for more severe cases of lymphedema.
In my case, I had 19 lymph nodes removed during surgery and 28 rounds of radiation. I first noticed something was off toward the end of radiation, when two of my fingers started to swell. It was only noticeable to me, but after several doctor visits, we finally confirmed it was lymphedema. I was fitted with a compression sleeve, gauntlet and custom glove to try to keep the swelling at bay but with limited success despite regular exercise, PT and use of a lymphatic pump. For this reason, at the 4-year mark, I opted for the lymphovenous bypass surgery and am seeing improved results. I am encouraged by the innovations that are happening in lymphedema care. Hopefully, given this information, you are too.
Again, remember you’re not alone in this. Be proactive with your care providers and connect with other survivors for support through your cancer center, Facebook groups like Lymphedema related to Breast Cancer or other organizations such as The Breasties and Unite for Her. We are stronger together.
For a free lymphedema self-care and treatment guide, visit https://www.cancerrehabpt.com/free-resources.










1 comment
Hi Virginia, thank you for this very informative article. As a breast cancer survivor and lymphedema sufferer (16 years) I’m happy to see more attention placed on this horrible side effect from treatments for breast cancer. I wish there was a cure. My life since breast cancer has completely changed my life – no more going to the beach or sitting by the pool, always worrying about a small nick on my arm or a bug bite. I have suffered many cellulitis infections, often requiring a hospital stay. I have much difficulty finding clothes to fit and can’t buy many top styles because they simply can’t fit my arm (even if I try a larger size). The general population has no clue as to how lymphedema impacts ones life.
I’m so lucky that I have had the same lymphedema physical therapist for the past 15 years. She has been wonderful but I know sooner or later she will retire and then I’ll have to find a new therapist which scares me since Lymphedema therapists are not easy to find.
Thank you for your very informative article!
I wish for a cure – we need a cure!
Leave a comment